Workers’ Compensation fraud has made regular appearances in the news lately. The impact of fraud in the system has become a forefront discussion with legislators and risk managers alike. Workers’ Compensation fraud is further exacerbated by an aging workforce and the rising cost of healthcare.
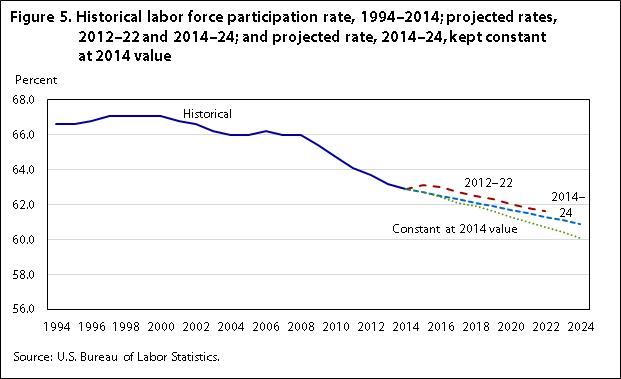
Today, the United States workforce is facing both an aging workforce and an increasing labor shortage. As more and more baby boomers retire and population growth slows, the labor force growth rate has hit an all-time low according to the U.S. Department of Labor. The labor force grew at 2.5 to 3 percent in the 1970s and the 1980s; 1.8 percent in the 1990s; 1.3 percent in 2000-2009; but grew only 0.5 percent in the last decade. According to the Wall Street Journal, a shrinking talent pool is one of the top concerns for corporate leaders in 2018 (Fuhrmans 2018). The insufficient growth rate will further stress the system since it is getting harder for employers to meet their hiring demands. With the labor shortage worsening, employers are forced to relax their hiring standards and recruit outside their usual talent pool by hiring inexperienced workers that may otherwise be unqualified. The labor shortfall will no doubt affect the workers’ compensation industry and lead to more claims, including fraudulent ones.
Compounding the issue is the rise of healthcare cost. Gone are the days when average healthcare deductibles were in the $500 to $1,000 range. Today, it is not uncommon for deductibles to hit anywhere from $3,000 to $10,000. This new reality has forced many people to ignore their condition or fraudulently claim that their injuries are work related – especially soft tissue injuries.
While you cannot control the actions of your employees, as an employer you can control your hiring practices. Hiring a good Third Party Administrator, therefore, makes a huge difference in one’s effort to curtail Workers’ Compensation fraud. At TRISTAR our staff has extensive criminal fraud investigation experience and have routinely identified and reported on suspected fraud. According to Probe Information Services, Inc., TRISTAR’s strategic business partner (SBP) for Investigation management, TRISTAR has a conviction rate of 90% for felony charges brought against fraudulent workers’ compensation claimants.
Due to the fact Workers’ Compensation claims are more susceptible to fraud not only from claimants, but also from medical providers, hospitals, out-patient surgery clinics, pharmacists and drug companies, TRISTAR must always be watchful for potential fraud in all transactions. We address this situation with a 3-pronged approach.
- First, we only work with SBP’s that adhere to the most stringent regulations and best practices when it comes to fraud prevention.
- Second, we have put in place antifraud programs that flag suspected abuse by using data to identify trends and monitor patterns, as well as investigative work related to social media monitoring. We routinely audit vendor payments for irregularities that could be a sign of fraudulent activities. When appropriate we report suspected fraud to State, local or in some cases federal law enforcement. This is known as “black box” auditing and includes responding to law enforcement demands for information relative to active law enforcement investigations and prosecutions.
- Last, we ensure that all our claims adjusters have had thorough background checks, receive continuing education and maintain current licenses for all states in which they are handling claims.
TRISTAR’s fraud prevention program is one of the many value added services we provide.
Works Cited
Bureau of Labor Statistics. Labor force projection to 2024. Decemeber 2015. https://www.bls.gov/opub/mlr/2015/article/labor-force-projections-to-2024.htm (accessed March 2019).
Fuhrmans, Joann S. Lublin and Vanessa. "Hackers and Shrinking Talent Pool Top CEO Concerns for 2018." The Wall Street Journal, 2018.